Introduction
Navigating the complex landscape of medical device development presents significant challenges due to stringent regulations and high stakes. As the healthcare industry continues to evolve, understanding the essential steps in this intricate process is crucial for innovators aiming to bring their ideas to market successfully. Identifying the key phases that influence a medical device's journey from concept to compliance is essential. This guide examines the critical stages of medical device development, providing insights and strategies to improve project management, ensure compliance, and enhance patient safety.
Understand the Medical Device Development Lifecycle
Navigating the medical equipment development process is fraught with challenges that require careful attention to each critical phase.
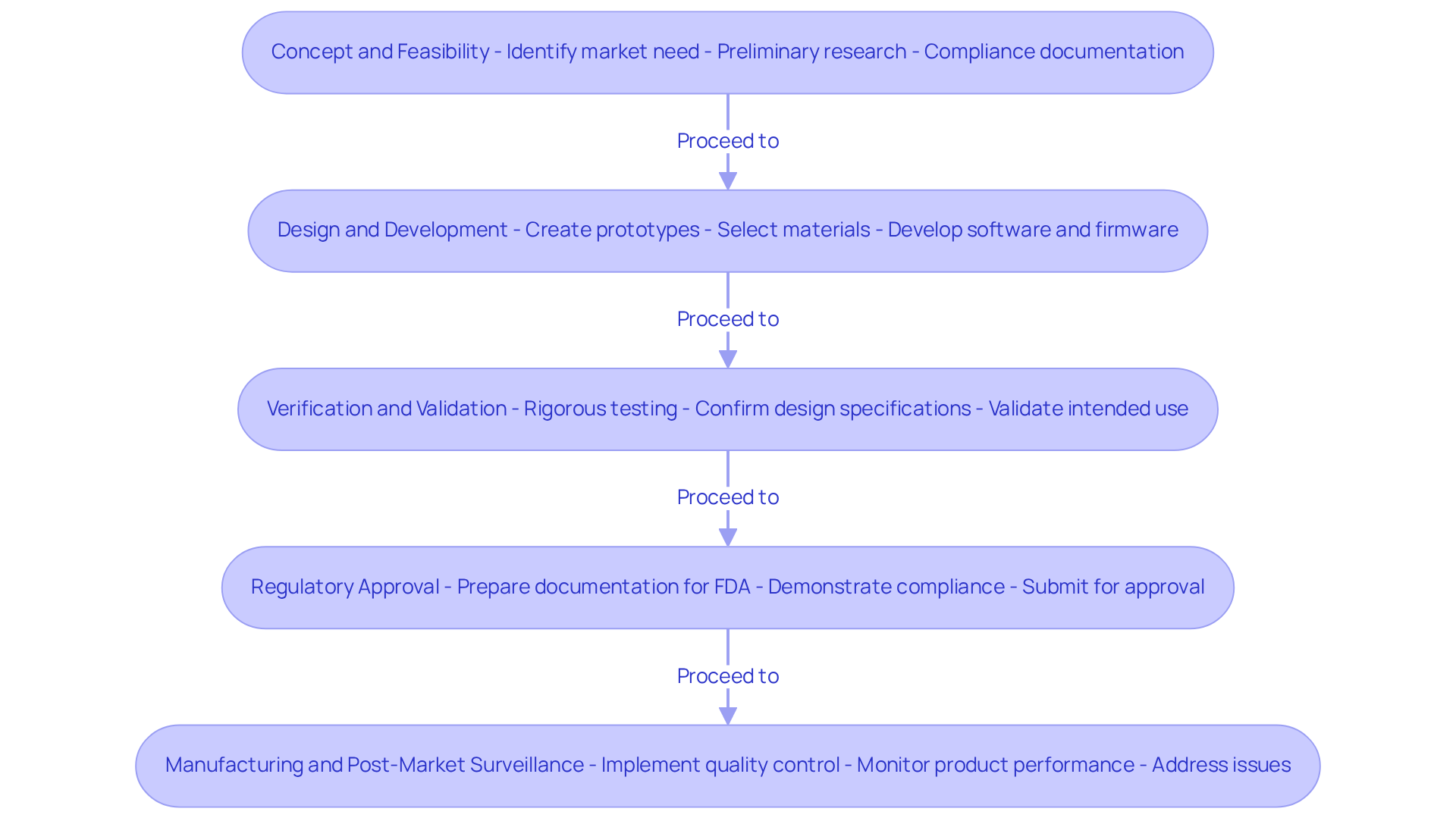
- Concept and Feasibility: This initial phase focuses on identifying a market need and brainstorming potential solutions. Conduct thorough preliminary research to assess the feasibility of your idea, considering technical, legal, and financial aspects. During this phase, Voler Systems offers crucial assistance with documentation compliance, providing insights on legal requirements and market analysis. This support is particularly important, given that a significant percentage of medical instruments do not succeed in development.
- Design and Development: Once the concept is validated, the next step is detailed design. This phase involves creating prototypes, selecting materials, and developing necessary software and firmware. It is essential to ensure that your design aligns with user needs and complies with regulatory requirements. Voler Systems assists in ensuring that all documentation, such as design history files and risk management plans, aligns with compliance standards, significantly enhancing patient outcomes.
- Verification and Validation: After creating the prototype, rigorous testing is conducted to confirm that the apparatus meets design specifications and validate its intended use. This step is crucial for ensuring safety and efficacy, as it directly impacts the device's market readiness. Documentation compliance during this phase includes test protocols and reports that support the validation procedure.
- Regulatory Approval: Prepare and submit comprehensive documentation to regulatory bodies, such as the FDA, for approval. This includes demonstrating compliance with applicable standards and regulations, which is vital for successful market entry. Voler Systems specializes in guiding startups through this complex process, ensuring that all necessary documentation, including 510(k) submissions and clinical evaluation reports, is thorough and accurate.
- Manufacturing and Post-Market Surveillance: Once approved, the focus shifts to manufacturing. Implement stringent quality control measures and establish a post-market surveillance plan to monitor the product's performance in real-world settings. Voler Systems continues to provide support in maintaining compliance and documentation throughout the product's lifecycle, including adverse event reporting and periodic safety updates.
Understanding these phases not only enhances the likelihood of success but also mitigates the risks associated with the development process of medical devices.
Identify Regulatory Compliance Requirements
To navigate the complexities of medical device regulations effectively, it is crucial to follow a structured approach:
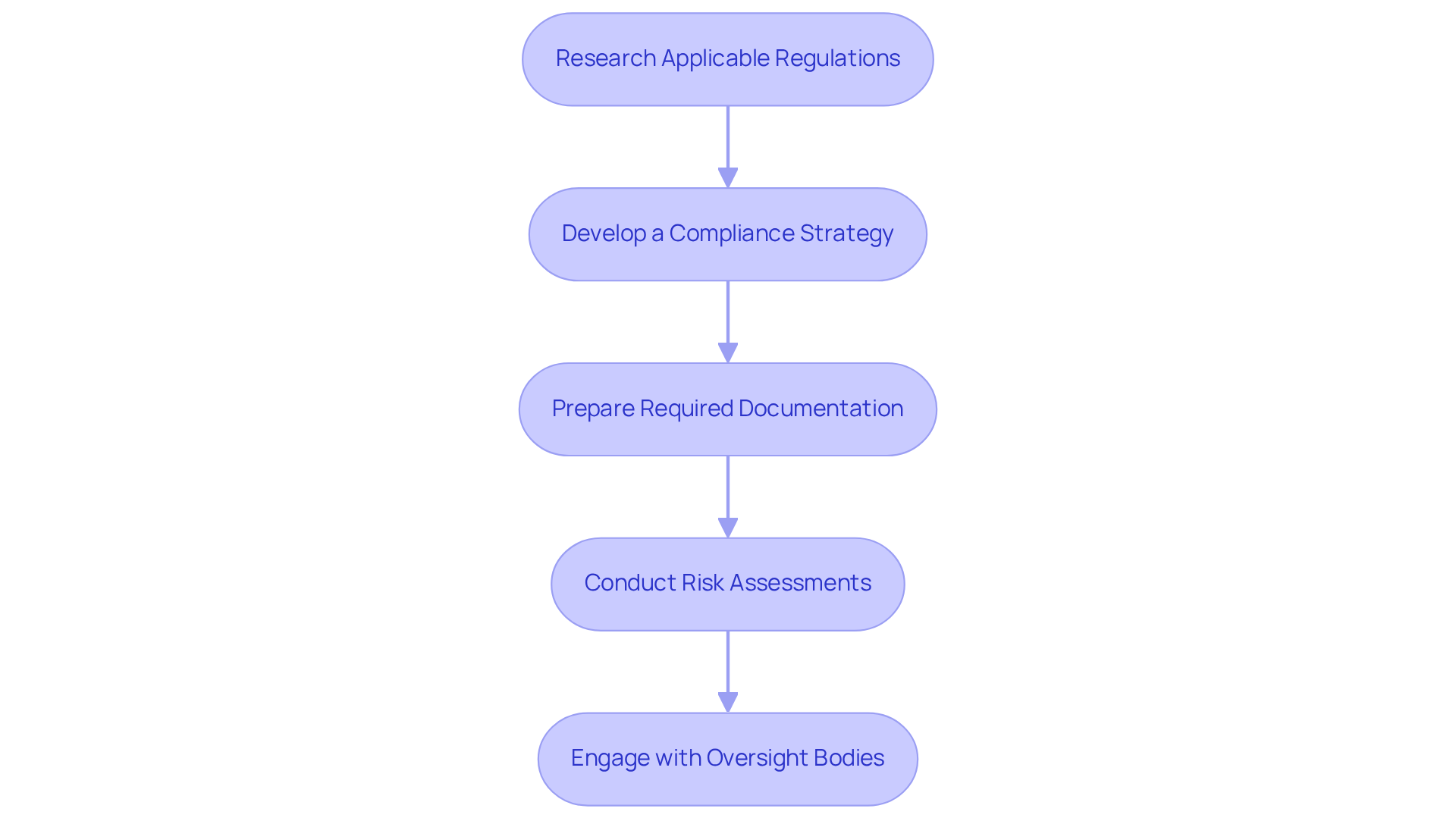
- Research Applicable Regulations: Identify the regulations that pertain to your equipment based on its classification (Class I, II, or III). Familiarize yourself with FDA guidelines, ISO standards, and any other relevant local or international regulations. Notably, as of 2026, the FDA has implemented new guidelines that emphasize the importance of cybersecurity in medical devices, making it essential to stay updated on these changes.
- Develop a Compliance Strategy: Create a compliance strategy that outlines the pathway to adherence. This should include timelines, required documentation, and testing protocols. Effective oversight strategies typically use Regulatory Information Management Systems (RIMS) to streamline compliance processes and ensure timely submissions.
- Prepare Required Documentation: Compile necessary documents such as the Design History File (DHF), Device Master Record (DMR), and Technical File. Ensure that all documentation is thorough and precise, as it will be examined by oversight authorities. Research indicates that approximately 70% of medical instruments achieve compliance on their first submission when documentation is well-organized.
- Conduct Risk Assessments: Perform risk assessments in accordance with ISO 14971 to identify potential hazards associated with your device and implement risk management strategies. This proactive approach is essential, particularly with the changing governance environment that mandates comprehensive risk management throughout the development process of the product lifecycle. Voler Systems employs advanced risk management tools to ensure compliance and safety.
- Engage with Oversight Bodies: Engaging in pre-submission meetings with oversight bodies can help clarify expectations and provide valuable feedback on your submission strategy. This proactive involvement can significantly simplify the approval process and improve your comprehension of compliance expectations.
By thoroughly understanding and addressing compliance requirements, you can significantly reduce the risk of delays and ensure a smoother path to market. By prioritizing compliance, you not only enhance your device's market readiness but also safeguard patient safety and trust.
Plan and Manage Your Development Project
To effectively plan and manage your medical device development project, adhere to the following steps:
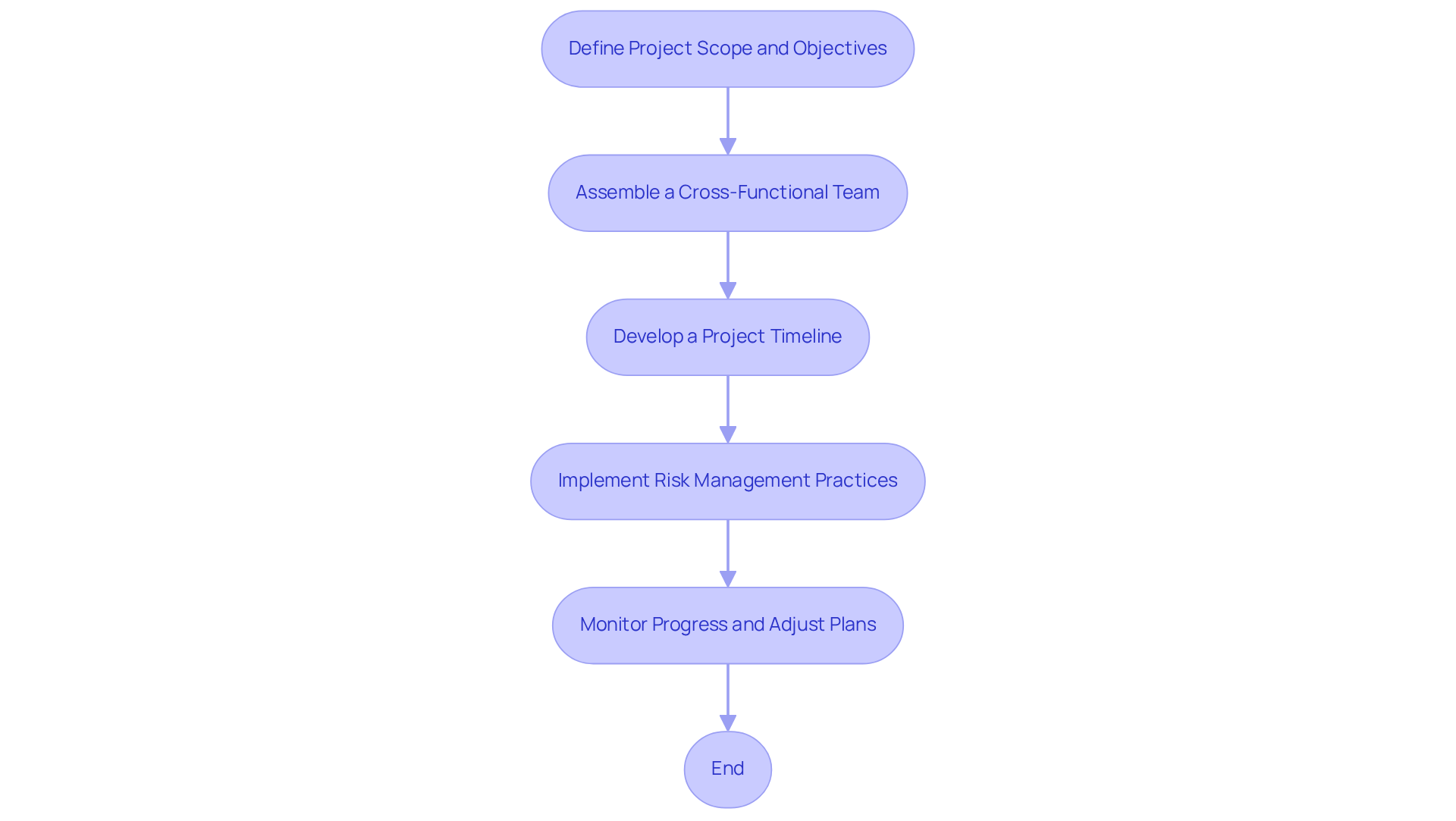
- Define Project Scope and Objectives: Clearly articulate the project scope, including specific goals, deliverables, and timelines. Establish measurable objectives to facilitate progress tracking.
- Assemble a Cross-Functional Team: Create a team with diverse expertise encompassing engineering, compliance, quality assurance, and marketing. Ensure all members understand their roles and responsibilities, fostering a collaborative environment.
- Develop a Project Timeline: Construct a detailed project timeline that encompasses all development phases, from concept to market launch. Utilize project management tools to visualize timelines and dependencies, ensuring clarity in the workflow.
- Implement Risk Management Practices: Identify potential risks at each development stage and devise mitigation strategies. Regularly review and update the risk management plan to adapt to project dynamics and emerging challenges. Identifying risks early can prevent costly setbacks later in the project.
- Monitor Progress and Adjust Plans: Continuously evaluate project progress against the established timeline and objectives. Be prepared to modify plans as necessary to address unforeseen challenges or changes in scope, ensuring alignment with regulatory requirements and market dynamics. Effective project management not only mitigates risks but also fosters innovation and efficiency.
By meticulously planning and managing your project, you enhance collaboration, streamline processes, and increase the likelihood of a successful development process for the product. A well-structured approach leads to innovative solutions that meet market needs and regulatory standards.
Implement Testing and Validation Protocols
To ensure the successful validation of your medical device, it is imperative to implement effective testing protocols:
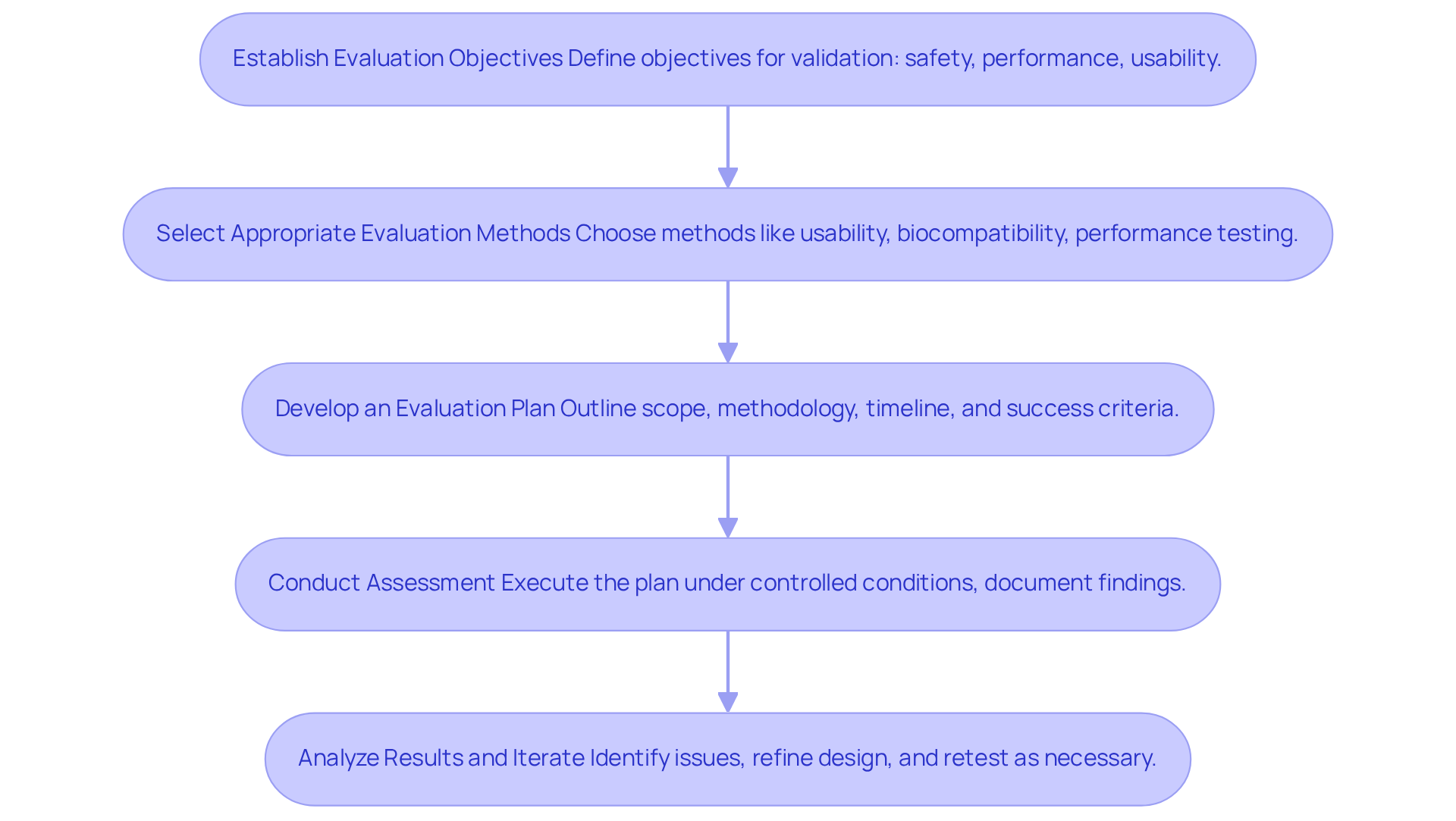
- Establish Evaluation Objectives: Clearly define the objectives of your assessment protocols, focusing on what you aim to validate, such as safety, performance, and usability.
- Select Appropriate Evaluation Methods: Choose evaluation methods that align with your objectives. Common methods include usability testing, biocompatibility testing, and performance testing. Ensure compliance with relevant standards, such as ISO 13485, to facilitate smoother regulatory processes. Robust test systems are essential for ensuring the quality and reliability of electronic device designs.
- Develop an Evaluation Plan: Create a comprehensive evaluation plan that outlines the scope, methodology, and timeline for each assessment. Include criteria for success and failure, along with data collection techniques to ensure comprehensive documentation, featuring user manuals that direct the assessment process.
- Conduct Assessment: Execute the evaluation plan under controlled conditions, meticulously documenting all findings. This data is essential for compliance submissions and demonstrates adherence to quality management standards.
- Analyze Results and Iterate: Analyze the results to identify issues or areas for improvement. Use this feedback to refine the design and retest as necessary, ensuring compliance and optimal performance.
In the development process, implementing comprehensive evaluation and validation protocols not only improves the safety and effectiveness of your medical product but also greatly boosts the chances of succeeding in initial assessment phases. Many producers struggle with initial assessment phases, making robust evaluation protocols essential. By prioritizing these steps, you position your equipment for successful regulatory approval and market entry.
Starting February 2, 2026, the FDA will enforce Quality Management System Regulations (QMSR), emphasizing the need for strong evaluation protocols. Furthermore, including usability assessments is crucial, as it directly affects user experience and equipment effectiveness. Expert insights indicate that a well-organized testing strategy can greatly enhance compliance rates and overall product quality, in line with Voler Systems' dedication to assisting medical startups in navigating these regulatory environments.
Facilitate Manufacturing Transfer and Production
To achieve a seamless manufacturing transfer and production process for your medical device, it is essential to follow a structured approach:
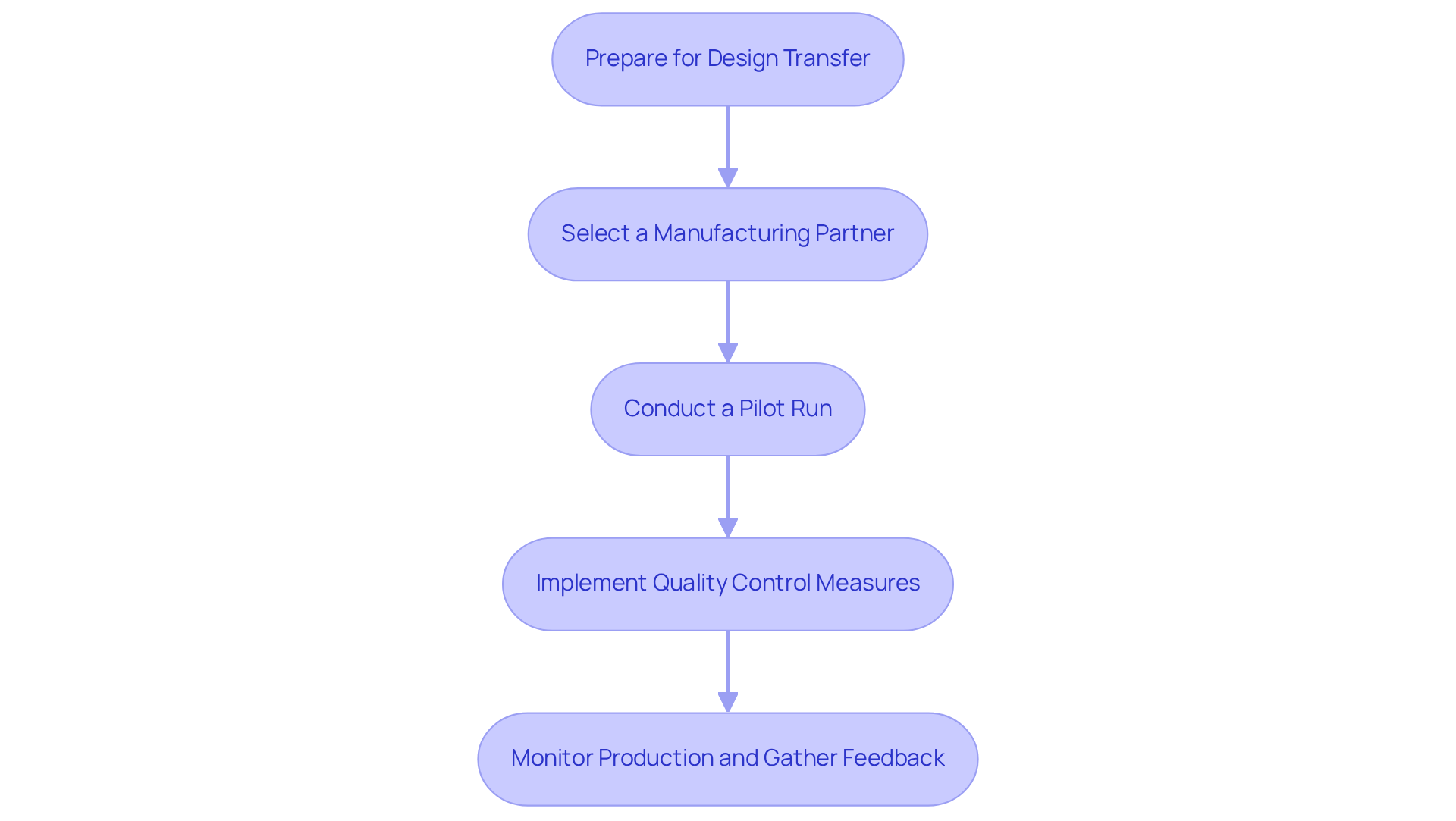
- Prepare for Design Transfer: Ensure that all design documentation is complete and accurate, including specifications, drawings, and manufacturing instructions that will guide the production process. This step is vital in the development process to reduce manufacturing errors.
- Select a Manufacturing Partner: Choose a manufacturing partner with proven experience in medical device production. Evaluate their capabilities, quality management systems, and adherence to standards, such as ISO 13485 certification. A knowledgeable partner can significantly impact your project's success throughout the development process by ensuring compliance with regulatory expectations and quality benchmarks.
- Conduct a Pilot Run: Before increasing production, carry out a pilot run to identify potential issues in the manufacturing system. This step enables the refinement of the development process and the establishment of effective quality control measures. Successful pilot runs can serve as a model for full-scale production, ensuring that any challenges are addressed early.
- In the development process, implement quality control measures such as regular inspections and testing to ensure production quality. Recording all qualification procedures, including Installation Qualification (IQ), Operational Qualification (OQ), and Performance Qualification (PQ), assists in upholding high standards throughout production.
- Monitor Production and Gather Feedback: Continuously monitor production and collect feedback from the manufacturing team. Key performance indicators (KPIs) such as yield, non-conformance rate, and on-time delivery performance should be tracked to ensure efficiency and quality. Be prepared to make adjustments as necessary to optimize both production efficiency and product quality.
By prioritizing these steps, you not only enhance production efficiency but also safeguard the integrity and compliance of your medical device.
Conclusion
Mastering the medical device development process is not just beneficial; it is essential for the successful introduction of innovative healthcare solutions. By understanding the intricate phases, from initial concept and feasibility through to manufacturing and post-market surveillance, stakeholders can significantly enhance their chances of developing compliant, effective, and safe medical devices.
Key insights from the article highlight the importance of:
- Rigorous planning
- Thorough documentation
- Proactive engagement with regulatory bodies
Each phase, including design, testing, and validation, plays a critical role in navigating the complexities of regulatory compliance. Navigating the complexities of regulatory compliance can be challenging for many stakeholders, and failure to adopt these practices may lead to increased risks and delays in market entry. Furthermore, implementing robust project management practices and risk assessment strategies fosters collaboration and innovation. This approach also mitigates potential setbacks.
Embracing these best practices streamlines the development process and prioritizes patient safety and trust in medical technologies. As the landscape of medical device regulations continues to evolve, organizations that prioritize excellence in every stage of development will not only enhance their market position but also play a pivotal role in shaping the future of healthcare.
Frequently Asked Questions
What are the main phases of the medical device development lifecycle?
The main phases include Concept and Feasibility, Design and Development, Verification and Validation, Regulatory Approval, and Manufacturing and Post-Market Surveillance.
What is the focus of the Concept and Feasibility phase?
This phase focuses on identifying a market need, brainstorming potential solutions, and conducting preliminary research to assess the feasibility of the idea, considering technical, legal, and financial aspects.
How does Voler Systems assist during the Concept and Feasibility phase?
Voler Systems provides assistance with documentation compliance, legal requirements, and market analysis to enhance the chances of success in medical device development.
What activities are involved in the Design and Development phase?
This phase involves creating prototypes, selecting materials, and developing necessary software and firmware while ensuring the design aligns with user needs and complies with regulatory requirements.
What is the purpose of the Verification and Validation phase?
The purpose is to conduct rigorous testing to confirm that the device meets design specifications and validate its intended use, ensuring safety and efficacy before market readiness.
What documentation is required for Regulatory Approval?
Comprehensive documentation must be prepared and submitted to regulatory bodies, including compliance demonstrations, 510(k) submissions, and clinical evaluation reports.
How does Voler Systems support the Regulatory Approval process?
Voler Systems guides startups through the complex regulatory approval process, ensuring thorough and accurate documentation is submitted.
What is involved in the Manufacturing and Post-Market Surveillance phase?
This phase focuses on implementing quality control measures during manufacturing and establishing a post-market surveillance plan to monitor product performance in real-world settings.
What steps should be taken to ensure regulatory compliance for medical devices?
Steps include researching applicable regulations, developing a compliance strategy, preparing required documentation, conducting risk assessments, and engaging with oversight bodies.
Why is it important to stay updated on regulatory changes, such as those from the FDA?
It is crucial to stay updated because new guidelines, such as those emphasizing cybersecurity in medical devices, can significantly impact compliance and market readiness.
How can effective oversight strategies improve compliance processes?
Effective oversight strategies often utilize Regulatory Information Management Systems (RIMS) to streamline compliance processes and ensure timely submissions.
What is the significance of conducting risk assessments in medical device development?
Conducting risk assessments helps identify potential hazards and implement risk management strategies, which are essential for compliance and safety throughout the product lifecycle.
List of Sources
- Understand the Medical Device Development Lifecycle
- Medical Device Development: 5 Phases From Concept to Market (https://arterexmedical.com/5-phases-of-medical-device-development)
- The 6 Phases of Medical Device Development (https://goddardtech.com/news-insights/the-6-phases-of-medical-device-development)
- Medical Product Development Trends - 2026 | IDP (https://innovativedesignproducts.com/medical-product-development-trends-2026)
- The Medical Device Product Development Journey: A Phase-by-Phase Guide (https://openregulatory.com/articles/the-medical-device-product-development-journey-a-phase-by-phase-guide)
- MedTech Product Development Trends in 2026 (https://enlil.com/blog/medtech-product-development-trends-in-2026)
- Identify Regulatory Compliance Requirements
- Navigating Medical Device Compliance in 2026 (https://regdesk.co/blog/guide-to-regulatory-compliance-for-medical-devices)
- medacuity.com (https://medacuity.com/qmsr-compliance-2026-deadline)
- A QMSR State of Mind: FDA Adopts New Inspection Approach for Medical Devices as Quality Management System Regulation Takes Effect | Insights | Ropes & Gray LLP (https://ropesgray.com/en/insights/alerts/2026/02/a-qmsr-state-of-mind-fda-adopts-new-inspection-approach-for-medical-devices)
- FDA Implements Quality Management System Regulation for Medical Devices (https://aabb.org/news-resources/news/article/2026/02/04/fda-implements-quality-management-system-regulation-for-medical-devices)
- Plan and Manage Your Development Project
- The Power of Cross-Functional Teams in MedTech (https://linkedin.com/pulse/power-cross-functional-teams-medtech-dakota-welker-jm2uc)
- What’s New in MedTech in 2026 — And What It Means for Converge (https://linkedin.com/pulse/whats-new-medtech-2026-what-means-converge-lq2te)
- Top medtech trends to watch in 2026 (https://medtechdive.com/news/medtech-trends-outlook-2026/810902)
- How AI Is Actually Helping MedTech Teams Move Faster — Across Every Stage of Medical Device Development - MedCity News (https://medcitynews.com/2026/01/how-ai-is-actually-helping-medtech-teams-move-faster-across-every-stage-of-medical-device-development)
- Driving Compliance and Speed: Cross-Functional Team Management in Medical Device Development (R&D… (https://medium.com/@deniskatz.info/driving-compliance-and-speed-cross-functional-team-management-in-medical-device-development-r-d-22a41764ae9b)
- Implement Testing and Validation Protocols
- FDA Device Guidance Agenda: What to Watch in 2026 (https://hoganlovells.com/en/publications/fda-device-guidance-agenda-what-to-watch-in-2026)
- xtalks.com (https://xtalks.com/top-medical-device-regulations-to-watch-in-2026-4549)
- 2026 Medical Device Quality Trends (https://mastercontrol.com/gxp-lifeline/2026-medical-device-trends-quality-management)
- MedTech news roundup March 2026 (https://congenius.ch/medtech-news-march-2026)
- mpo-mag.com (https://mpo-mag.com/medical-device-testing-in-transition)
- Facilitate Manufacturing Transfer and Production
- Advice for medical device manufacturers in 2026 | Medical Economics (https://medicaleconomics.com/view/advice-for-medical-device-manufacturers-in-2026)
- mddionline.com (https://mddionline.com/medical-device-regulations/navigate-2026-s-medical-device-manufacturing-trends)
- Rediscovering Smiles: A Caregiver's Journey (https://swikmedical.com/finding-the-right-partner-how-inventors-can-navigate-medical-device-manufacturing)
- A Complete Guide to Medical Device Technology Transfer When Moving to a New CDMO - Arrotek | Medical Device Innovation (https://arrotek.com/a-complete-guide-to-medical-device-technology-transfer-when-moving-to-a-new-cdmo)






