Introduction
An effective Failure Mode and Effects Analysis (FMEA) is essential in the medical device industry, where patient safety and regulatory compliance are paramount. This guide outlines the step-by-step process for conducting an FMEA, providing insights into how manufacturers can identify potential errors, assess their impacts, and prioritize risks to improve product reliability. As regulatory standards continue to evolve, organizations face a critical challenge: ensuring that their FMEA processes not only fulfill compliance requirements but also protect patients from potential device failures.
Understand FMEA in the Context of Medical Devices
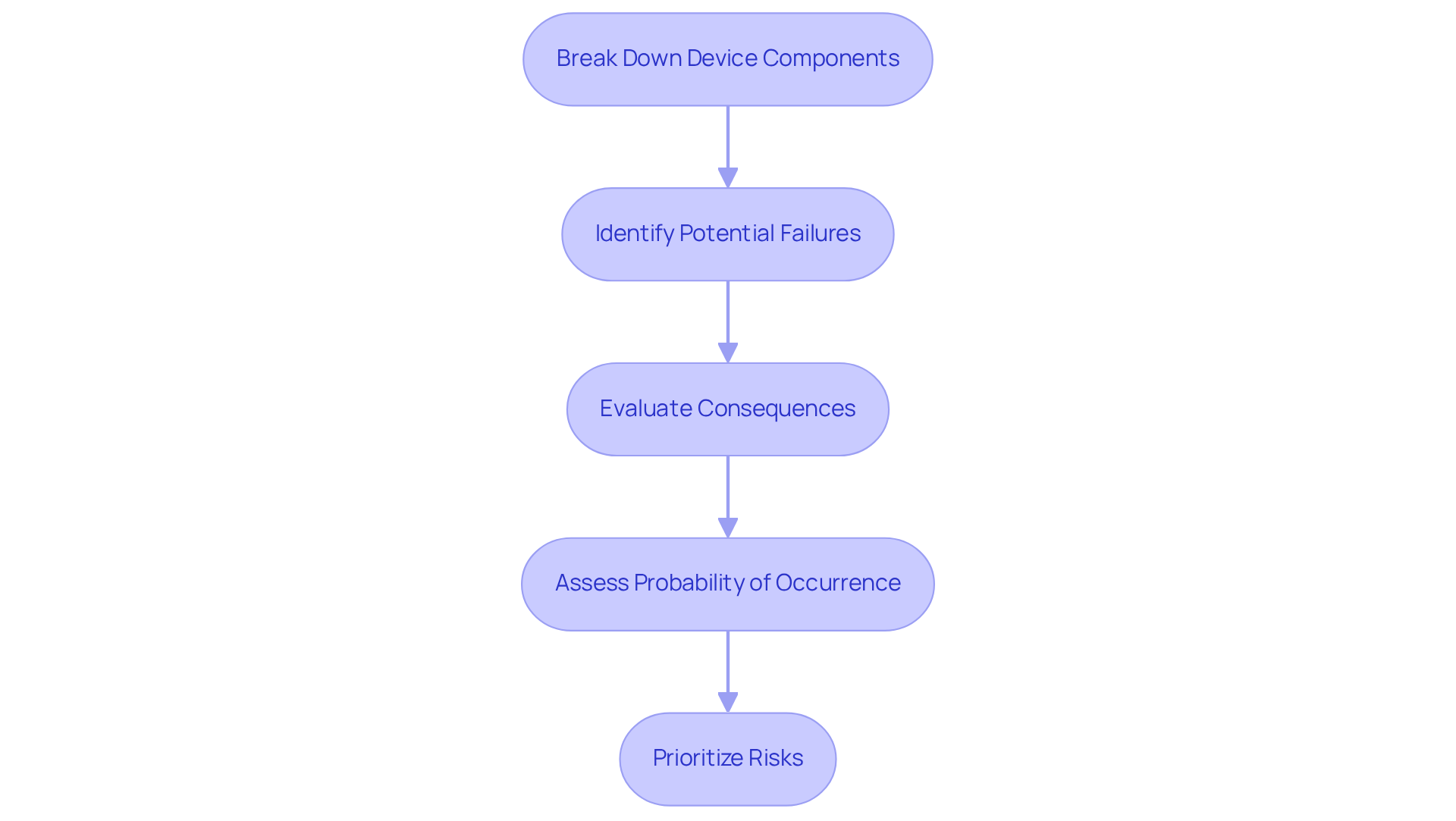
An illustrates an essential, organized approach for identifying potential errors in , evaluating their impacts, and prioritizing them based on severity and likelihood. This process is particularly critical for set for 2026, as it directly affects . By breaking down a device into its components, FMEA assesses how each part may fail, the potential consequences of these failures, and their probabilities of occurrence. This proactive tool, which serves as an , not only identifies risks but also aids in developing before can arise.
The practical applications of have demonstrated significant improvements in . For instance, in the development of , an has been instrumental in identifying that could lead to inaccurate readings, thereby ensuring that devices provide reliable data for patient monitoring. Moreover, as regulatory scrutiny intensifies - especially with the FDA's focus on - FMEA serves as a foundational element for manufacturers to demonstrate compliance and enhance the safety profile of their products. Data indicates that organizations employing FMEA effectively reduce the incidence of device-related , underscoring its importance in the realm of medical device safety.
Conduct Step-by-Step FMEA Analysis
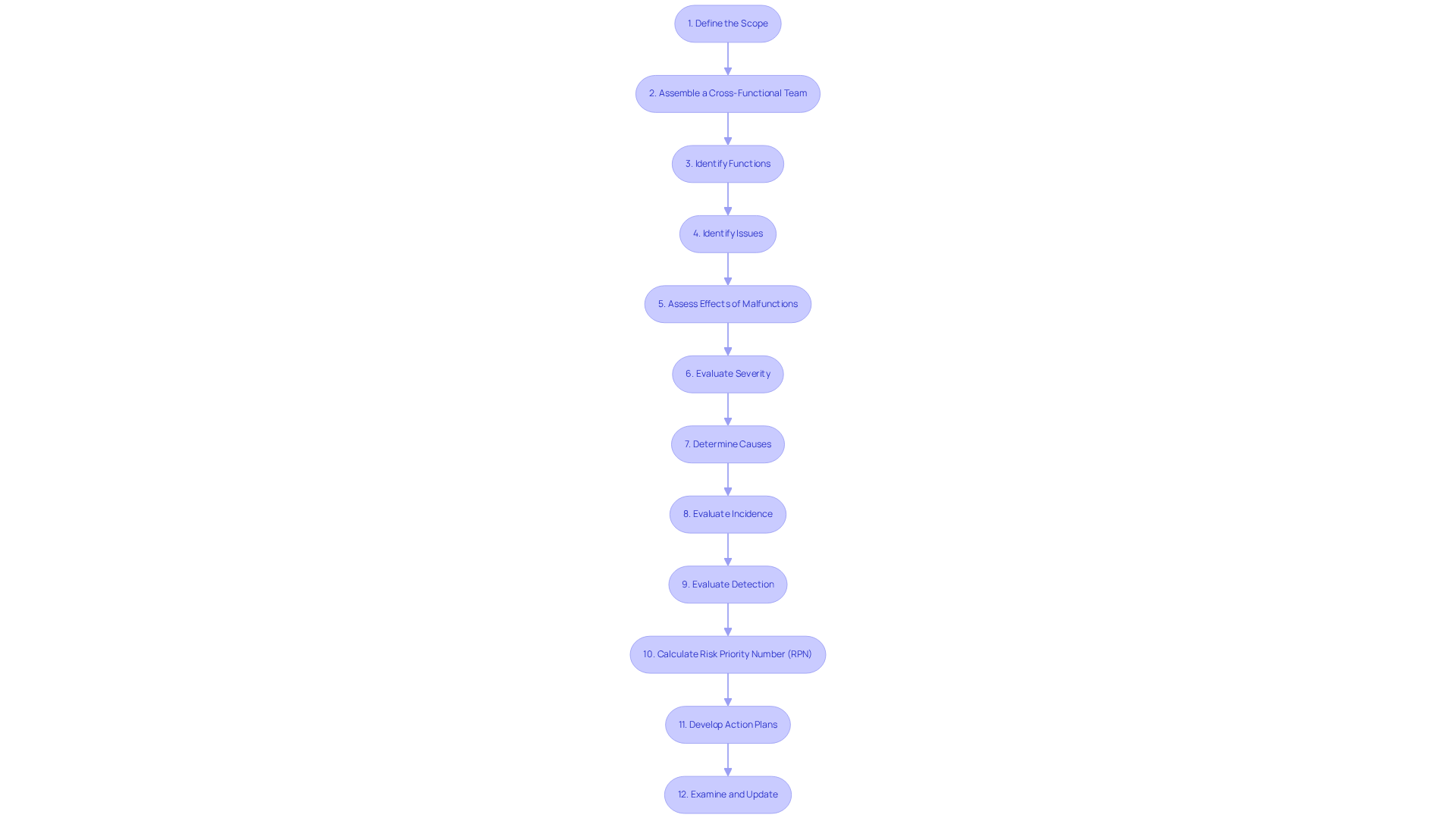
- Define the Scope: Clearly outline the system, subsystem, or component under analysis, specifying the boundaries to focus on pertinent .
- Assemble a : Gather a diverse team with expertise in engineering, quality assurance, regulatory affairs, and other relevant fields. This collaboration ensures comprehensive input and enhances the .
- Identify Functions: List the functions of the device or component being analyzed. Understanding the intended functions of each component is essential for recognizing possible issues.
- Identify Issues: For each function, brainstorm possible problems. Consider how each component could fail to perform its intended function, drawing on insights from various team members.
- Assess Effects of Malfunctions: Determine the potential impacts of each malfunction mode on device performance and . This step is critical for effectively prioritizing risks in an .
- Evaluate Severity: Rate the severity of each effect on a scale (e.g., 1 to 10), where 10 represents a catastrophic incident that could lead to serious injury or death.
- Determine Causes: Identify the underlying reasons for each malfunction. Understanding why a setback might occur is essential for developing effective mitigation strategies, as illustrated by the .
- Evaluate Incidence: Gauge the probability of each malfunction type occurring, employing a scale to quantify the risk and aid in prioritization.
- : Assess the capability to identify each error type before it affects the patient. This evaluation helps understand the effectiveness of current controls and informs necessary improvements.
- Calculate Risk Priority Number (RPN): Multiply the severity, occurrence, and detection ratings to obtain the RPN for each failure mode. This number assists in prioritizing which threats need immediate attention in an .
- Develop : For high-priority threats, create to reduce or eliminate these challenges. This may involve , additional testing, or enhanced monitoring protocols, addressing common errors in manufacturing tests to ensure quality and efficiency.
- Examine and Update: Regularly assess the as the design progresses or new data emerges, ensuring it remains a dynamic document that accurately represents current risks and controls.
Document and Review FMEA Findings for Compliance
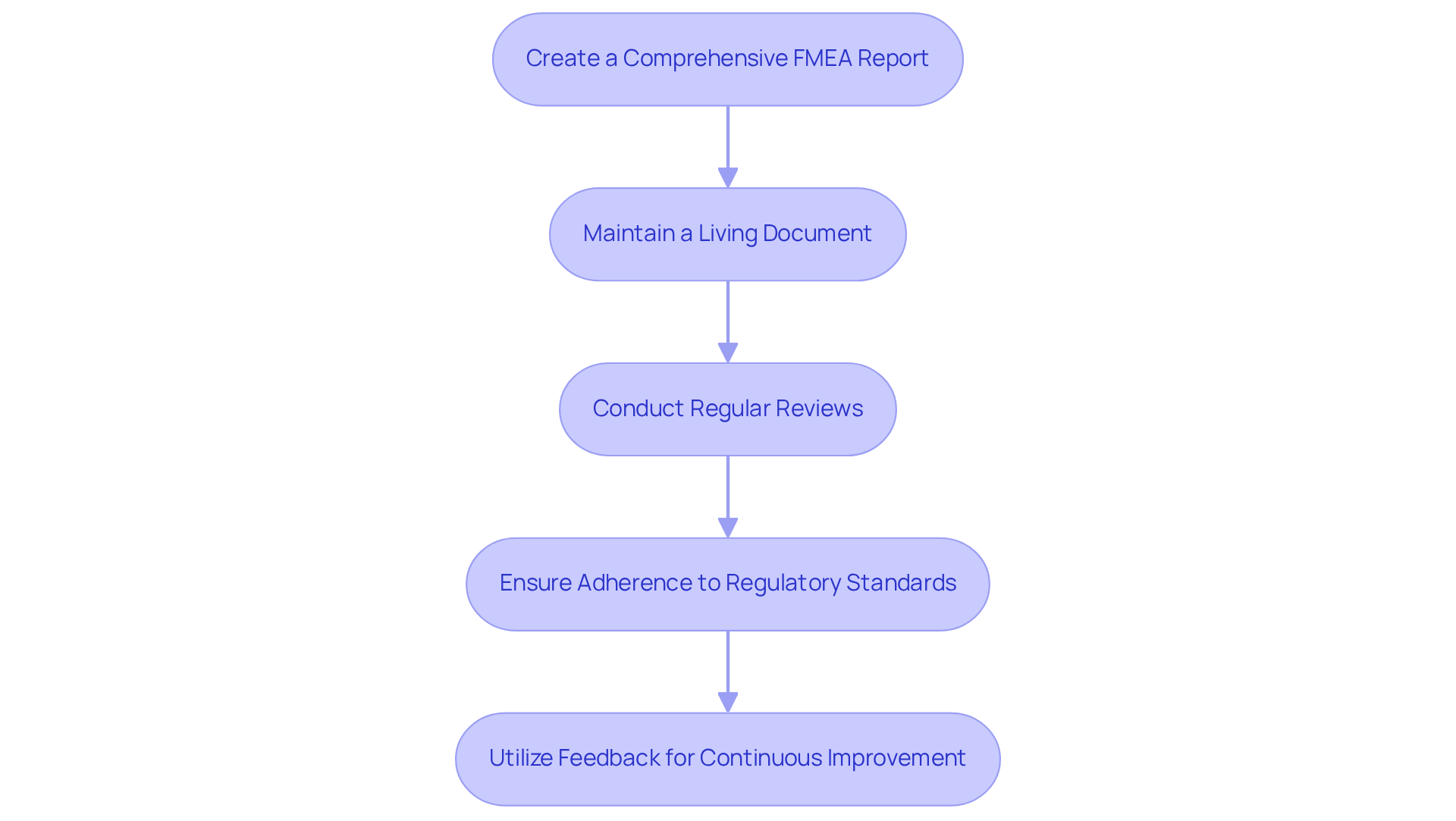
- Create a Comprehensive Report: Document all findings meticulously, including identified failure modes, their effects, causes, and calculated Risk Priority Numbers (RPNs). Ensure clarity and accessibility for all stakeholders involved in the development process.
- Maintain a : Treat the as a dynamic entity that requires regular updates as new information surfaces or design modifications occur. This practice ensures that the analysis remains pertinent and reflective of the current state of the project.
- : Arrange periodic evaluations of the failure modes and effects analysis with a cross-departmental team to assess the efficacy of executed actions and to recognize any new threats. This collaborative approach fosters a proactive risk management culture.
- Ensure Adherence to : Acquaint yourself with relevant regulations, such as , and confirm that your documentation aligns with these requirements. This alignment is essential for , particularly with the , effective February 2, 2026.
- Utilize Feedback for : Actively encourage team members to provide insights on the failure modes and effects analysis process and findings. Leveraging this feedback can refine the analysis and enhance the quality of future FMEAs, ultimately contributing to better .
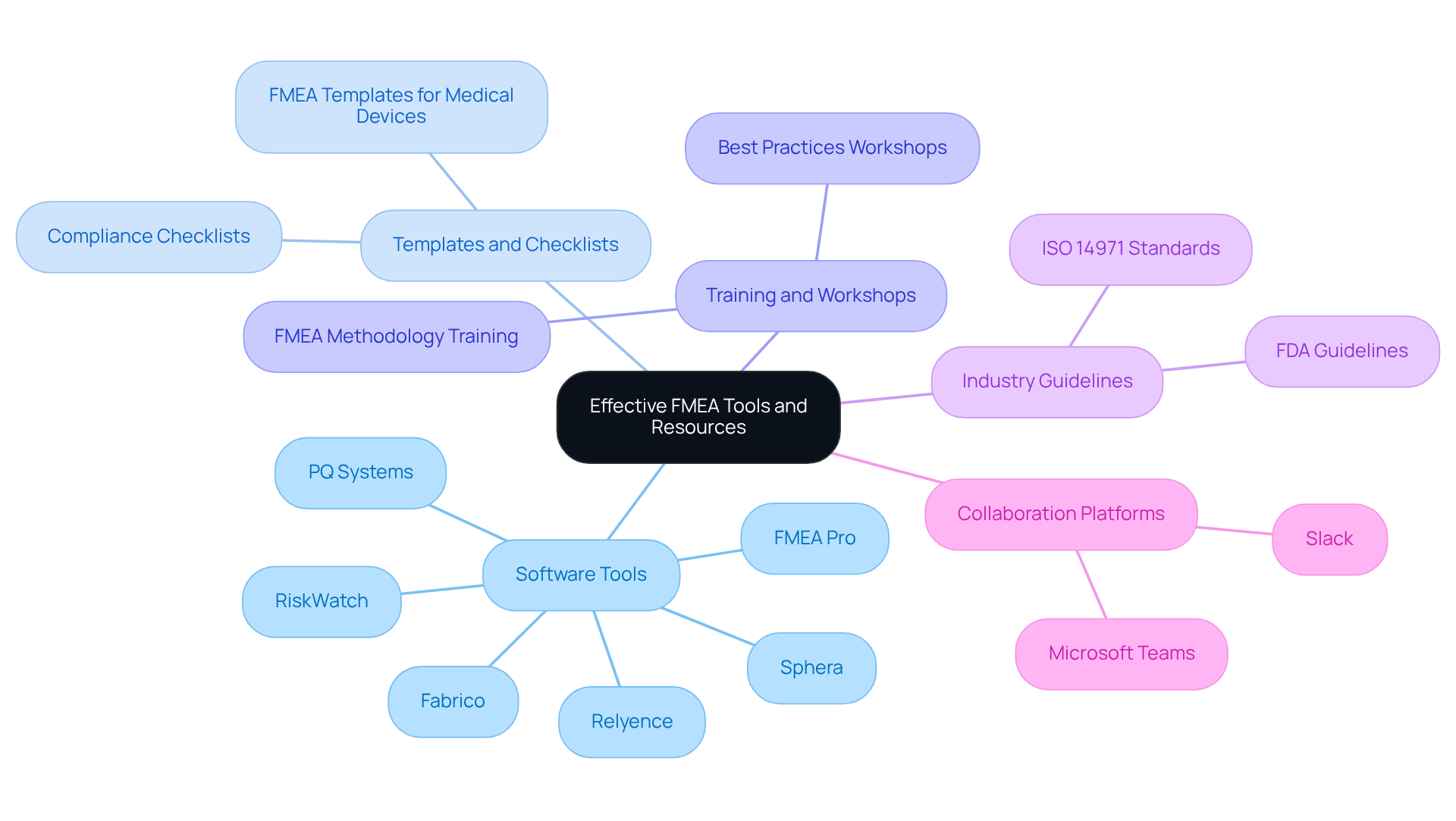
- : Employ specialized software such as RiskWatch or FMEA Pro to streamline the analysis process. These tools facilitate collaboration, maintain thorough documentation, and ensure that analyses are both comprehensive and actionable.
- : Adopt and checklists specifically designed for medical device compliance in 2026. These resources standardize the process, ensuring that critical steps are not overlooked and significantly enhancing the effectiveness of . Research indicates that well-organized templates substantially improve the reliability of results.
- : Allocate resources to comprehensive training programs for team members on failure mode and effects analysis methodologies and best practices. Workshops not only deepen understanding but also enhance the , fostering a culture of continuous improvement in risk management.
- Industry Guidelines: Adhere to , such as those established by the FDA and ISO, which delineate best practices for conducting failure mode and effects analysis. These documents offer essential insights into regulatory expectations and assist in ensuring compliance with evolving standards.
- Collaboration Platforms: Implement or Slack to improve communication among team members throughout the FMEA process. This strategy ensures that diverse perspectives are integrated into the analysis, ultimately enhancing the quality and comprehensiveness of the risk assessment.
Conclusion
Implementing an effective Failure Mode and Effects Analysis (FMEA) is essential for ensuring compliance and enhancing patient safety within the medical device industry. This structured approach identifies potential risks and prioritizes them based on severity and likelihood of occurrence. By systematically evaluating each component of a medical device, manufacturers can proactively address vulnerabilities, thereby safeguarding patient health and adhering to stringent regulatory standards.
The article outlines key steps in conducting an FMEA, including:
- Defining the scope
- Assembling a cross-functional team
- Identifying functions and issues
- Assessing effects and severity
- Developing actionable plans
The importance of maintaining a living document that is regularly updated and reviewed is emphasized, ensuring that the FMEA remains relevant as designs evolve and new data emerges. Utilizing specialized tools, templates, and continuous training further enhances the effectiveness of the FMEA process, enabling organizations to cultivate a culture of risk management and compliance.
In conclusion, the implementation of a thorough FMEA process not only aligns with regulatory requirements but also plays a vital role in advancing the quality and safety of medical devices. As the landscape of medical device regulations continues to evolve, embracing these best practices is essential for manufacturers aiming to mitigate risks and improve patient outcomes. By prioritizing FMEA, organizations can contribute to a safer healthcare environment and demonstrate their commitment to excellence in medical device compliance.
Frequently Asked Questions
What is FMEA in the context of medical devices?
FMEA, or Failure Mode and Effects Analysis, is an organized approach for identifying potential errors in medical devices, evaluating their impacts, and prioritizing them based on severity and likelihood.
Why is FMEA important for medical devices?
FMEA is crucial for compliance with evolving regulatory standards set for 2026, as it directly impacts patient safety by identifying risks and helping to develop effective mitigation strategies.
How does FMEA work in assessing medical devices?
FMEA breaks down a device into its components to assess how each part may fail, the potential consequences of these failures, and their probabilities of occurrence.
What are the practical applications of FMEA in medical devices?
FMEA has shown significant improvements in patient safety, such as in the development of wearable health monitors, by identifying key failure points that could lead to inaccurate readings.
How does FMEA relate to regulatory compliance?
As regulatory scrutiny increases, especially from the FDA regarding risk management, FMEA serves as a foundational element for manufacturers to demonstrate compliance and enhance the safety profile of their products.
What impact does FMEA have on adverse events related to medical devices?
Organizations that effectively employ FMEA have been shown to reduce the incidence of device-related adverse events, highlighting its importance in medical device safety.
List of Sources
- Understand FMEA in the Context of Medical Devices
- The medical device trends doctors can expect to see in 2026 | Medical Economics (https://medicaleconomics.com/view/the-medical-device-trends-doctors-can-expect-to-see-in-2026)
- FDA's Risk Management Expectations for Medical Devices: What Manufacturers Need to Know (https://gardner.law/news/fda-risk-management-expectations-medical-devices)
- Christina Bergeron Previews Regulatory Risk Factors in 2026 for Medical Device Targets in Trending Video | News & Events | Ropes & Gray LLP (https://ropesgray.com/en/news-and-events/news/2026/02/christina-bergeron-previews-2026-medical-device-targets-in-trending-video)
- Velocity 360 USA Training (https://velocity360training.com/pages/blog?p=a-new-era-of-medical-device-quality-is-your-medical-device-qms-built-to-face-a-global-future)
- How Will FDA's New Rules Impact Your Health Gadgets? (https://spectrum.ieee.org/fda-medical-device-rules)
- Conduct Step-by-Step FMEA Analysis
- FDA Device Guidance Agenda: What to Watch in 2026 (https://hoganlovells.com/en/publications/fda-device-guidance-agenda-what-to-watch-in-2026)
- The Medtech Landscape in 2026: Here’s What to Expect (https://mddionline.com/business/the-medtech-landscape-in-2026-here-s-what-to-expect)
- Christina Bergeron Previews Regulatory Risk Factors in 2026 for Medical Device Targets in Trending Video | News & Events | Ropes & Gray LLP (https://ropesgray.com/en/news-and-events/news/2026/02/christina-bergeron-previews-2026-medical-device-targets-in-trending-video)
- Failure Mode and Effects Analysis (FMEA) for Medical Devices (https://vem-medical.com/fmea-for-medical-devices)
- airacad.com (https://airacad.com/top-benefits-of-implementing-fmea-six-sigma-in-your-organization)
- Document and Review FMEA Findings for Compliance
- Velocity 360 USA Training (https://velocity360training.com/pages/blog?p=a-new-era-of-medical-device-quality-is-your-medical-device-qms-built-to-face-a-global-future)
- FDA Implements Quality Management System Regulation for Medical Devices (https://aabb.org/news-resources/news/article/2026/02/04/fda-implements-quality-management-system-regulation-for-medical-devices)
- QMSR: What the U.S. FDA’s New Inspection Manual Really Means for Device Manufacturers (https://emergobyul.com/news/qmsr-what-us-fdas-new-inspection-manual-really-means-device-manufacturers)
- FDA Aligns U.S. Medical Device Rules with Global Standards (https://mddionline.com/regulatory-quality/medical-device-companies-must-navigate-historic-fda-rule-change)
- A QMSR State of Mind: FDA Adopts New Inspection Approach for Medical Devices as Quality Management System Regulation Takes Effect | Insights | Ropes & Gray LLP (https://ropesgray.com/en/insights/alerts/2026/02/a-qmsr-state-of-mind-fda-adopts-new-inspection-approach-for-medical-devices)
- Utilize Tools and Resources for Effective FMEA
- Failure mode effect analysis use and limitations in medical device risk management (https://sciencedirect.com/science/article/pii/S2199853124002336)
- 5 Best FMEA Software Tools for Reliability (2026 Review) (https://fabrico.io/blog/best-fmea-software-tools)
- FDA Digital Health Guidance: 2026 Requirements Overview | IntuitionLabs (https://intuitionlabs.ai/articles/fda-digital-health-technology-guidance-requirements)
- Best 12+ Medical Device Quality Management Tools for 2026 (https://visuresolutions.com/medtech-and-pharma-guide/best-quality-management-tools)
- Cybersecurity: Quality System Considerations and Premarket Submissions (https://fda.gov/regulatory-information/search-fda-guidance-documents/cybersecurity-medical-devices-quality-management-system-considerations-and-content-premarket)





