Introduction
Navigating the complex landscape of medical device development necessitates a thorough understanding of best practices that not only ensure compliance but also enhance user experience. As the industry progresses, the integration of regulatory knowledge, user-centered design, and advanced technologies becomes essential for achieving success. Developers face the challenge of balancing innovation with compliance while addressing the diverse needs of users. This article explores four critical practices that can significantly enhance the development process and outcomes of new medical devices, paving the way for safer and more effective healthcare solutions.
Understand Regulatory Compliance Requirements
To successfully navigate the complex landscape of , understanding the that govern the industry is essential. The following key practices are crucial:
- Familiarize Yourself with Relevant Regulations: Begin by identifying the specific regulations applicable to your equipment, such as the or ISO 13485 for . A thorough comprehension of these regulations will guide your creation and development processes.
- : A DHF is a comprehensive document that records the creation and development process of a medical device. It should encompass design inputs, outputs, verification, and validation activities. Maintaining a well-structured DHF is vital for compliance submissions and audits.
- : Establishing communication with regulatory agencies early in the development process can yield valuable insights and clarify expectations. Consider scheduling pre-submission meetings to discuss your product and gather feedback.
- Implement Robust Design Controls: that ensure the device meets user needs and intended uses. This includes conducting risk assessments, design reviews, and verification and validation activities throughout the development process.
- : The oversight landscape is continually evolving. Regularly review updates from regulatory bodies and industry standards organizations to ensure ongoing compliance. This proactive approach can help mitigate risks associated with non-compliance.
Incorporate User-Centered Design Principles
(UCD) serves as a vital framework that emphasizes the needs, preferences, and limitations of end-users throughout the creation process. The following best practices effectively incorporate UCD in :
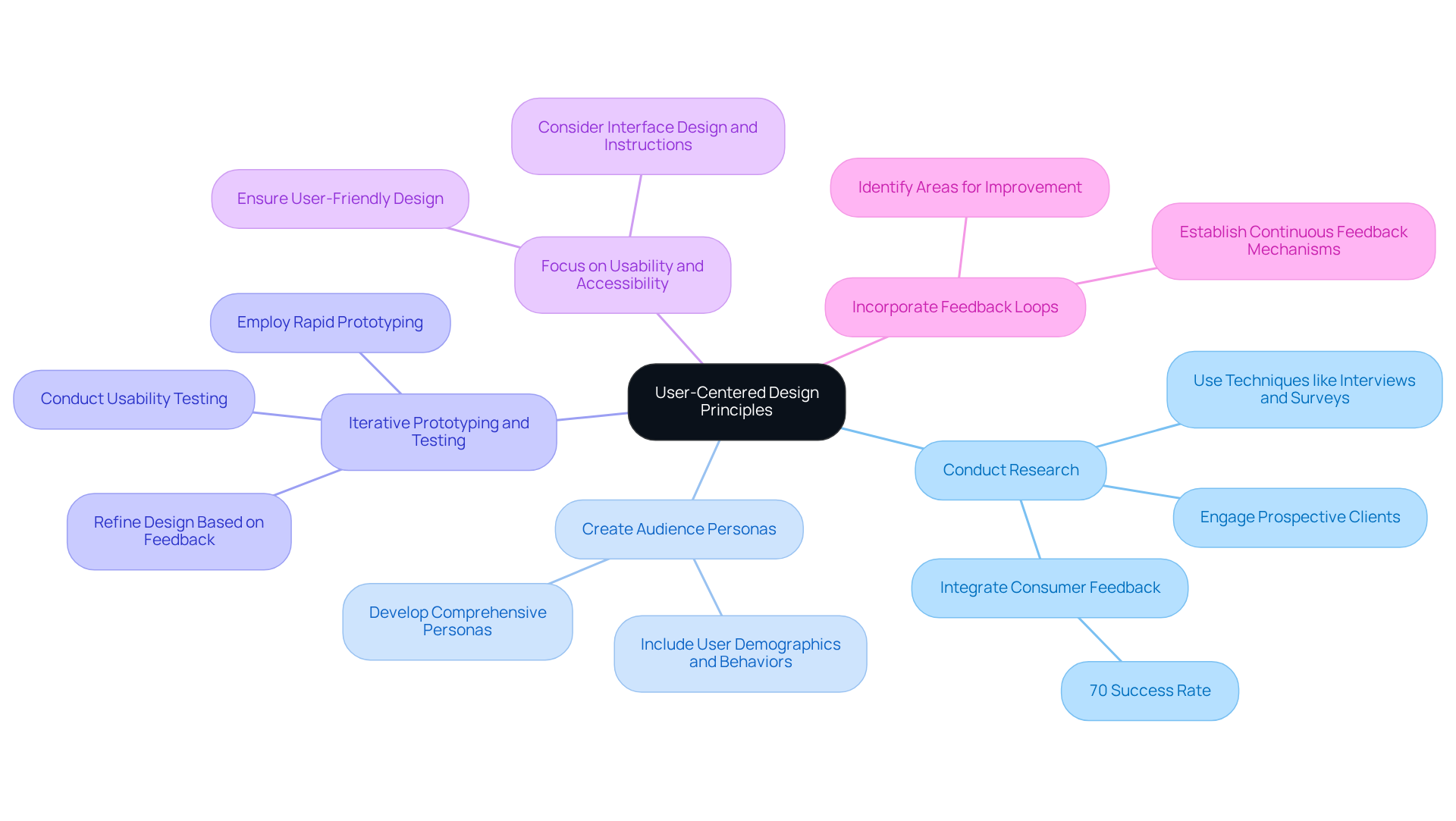
- Conduct Research: to gather insights regarding their needs, preferences, and challenges. Techniques such as interviews, surveys, and observational studies provide valuable data that inform development decisions. Research indicates that over 70% of successful medical products integrate during their creation, underscoring the critical importance of consumer involvement.
- Create Audience Personas: Develop comprehensive personas that represent the target demographic for your device. These personas should include user demographics, behaviors, and objectives, guiding decisions that resonate with actual users. This approach ensures that the creation process aligns with the real experiences and expectations of end-users.
- : Employ rapid prototyping to develop early versions of your product. to collect feedback and refine the design. This iterative process helps identify usability issues and enhances the product before final development, ensuring that it effectively meets the needs of its users.
- : Ensure that the device is and accessible to all potential users, including those with disabilities. Consider aspects such as interface design, labeling, and instructions to improve the user experience. A well-designed interface can significantly boost engagement and satisfaction, leading to improved clinical outcomes.
- : Establish mechanisms for continuous feedback from users even after the product launch. This practice aids in identifying areas for improvement and informs subsequent versions of the product, fostering a culture of ongoing enhancement based on user experiences. Consistent feedback can lead to innovations that align with evolving consumer needs and regulatory standards.
Leverage Advanced Technologies for Innovation
Integrating into medical equipment development can lead to significant improvements in functionality and user experience. Here are effective practices for leveraging technology:
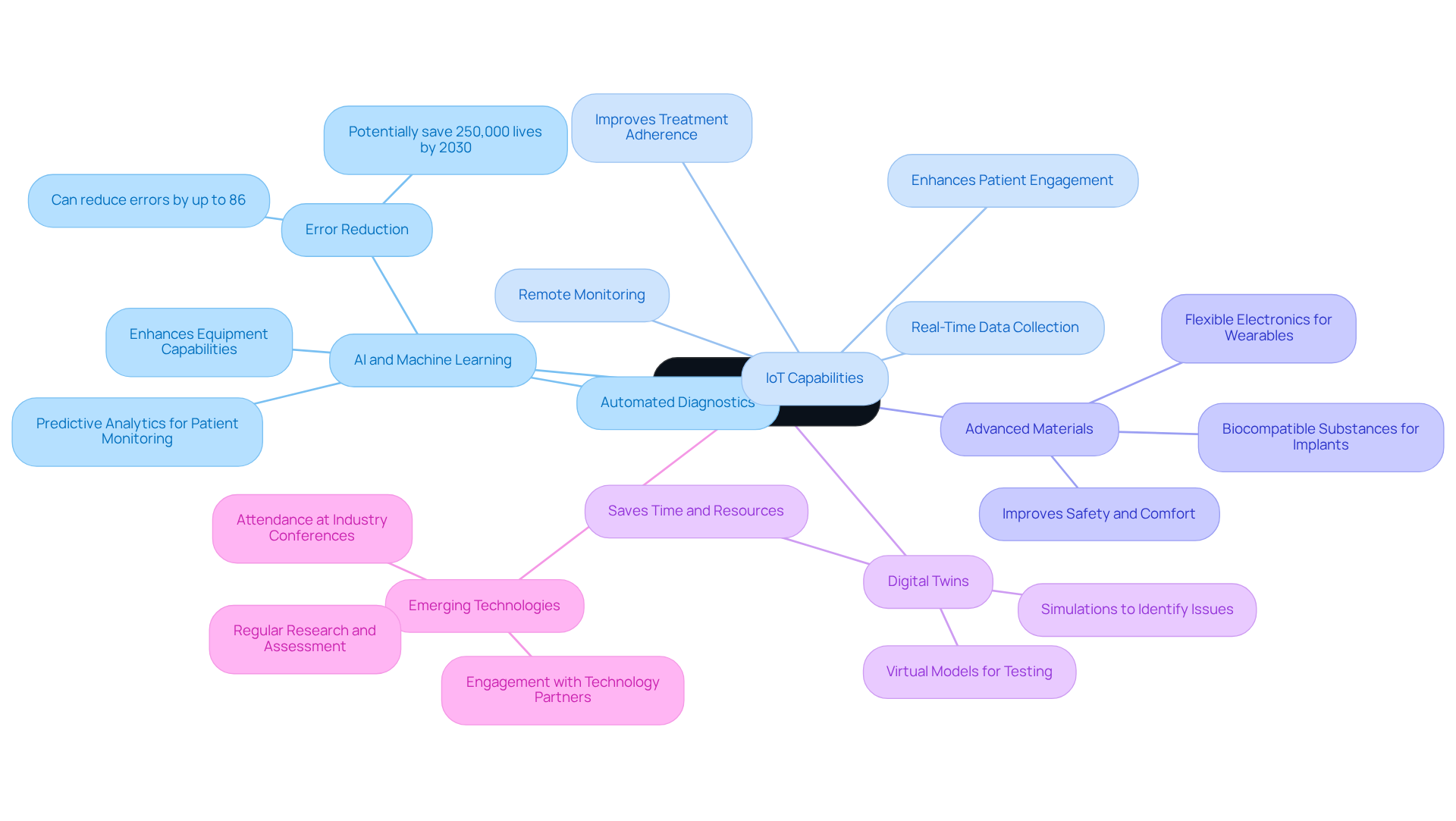
- Utilize : Implement to enhance equipment capabilities, such as or automated diagnostics. These technologies can , with studies indicating that AI can reduce errors by up to 86% and potentially save 250,000 lives by 2030.
- Integrate IoT Capabilities: Design instruments with features to enable . This connectivity enhances patient engagement, allowing healthcare providers to access valuable insights and improve care quality. Recent advancements in IoT have shown that devices equipped with these capabilities can significantly enhance patient adherence to treatment plans.
- : Explore the use of innovative materials that can enhance performance, such as biocompatible substances for implants or flexible electronics for wearables. These materials improve safety and user comfort, making products more appealing to both patients and healthcare professionals.
- Implement Digital Twins: Utilize to create virtual models of your apparatus for testing and optimization. This approach allows for simulations that can identify potential issues before physical prototypes are built, saving time and resources while ensuring compliance with regulatory standards.
- : Regularly research and assess new technologies that could enhance your product development process. Engaging with technology partners and attending industry conferences can provide insights into the latest advancements, ensuring your products remain competitive in a rapidly evolving market.
Conduct Comprehensive Testing and Validation
Thorough testing and validation are critical in the , ensuring safety, efficacy, and compliance. Here are best practices for conducting comprehensive testing:
- Develop a : Formulate a detailed that outlines the types of tests to be conducted, including functional, safety, usability, and compliance tests. This strategy should align with the equipment's intended purpose and legal standards, ensuring that all essential elements are addressed, including assistance with .
- Perform Risk Assessments: Conduct associated with the equipment. This process should utilize methodologies such as (FMEA) and Hazard Analysis, which help prioritize testing protocols based on the severity and likelihood of identified risks. Engaging trained professionals in is essential for thorough evaluations, especially in the context of integrating AI technologies that can enhance risk identification and mitigation.
- Utilize Standardized Testing Protocols: Adhere to established , such as and IEC 60601 for electrical safety. Following these standards not only streamlines the testing procedure but also enhances the credibility of the results, making them more acceptable to oversight authorities.
- Engage Third-Party Testing Labs: Collaborate with . This partnership can provide an impartial assessment of the device's performance and compliance with standards, which is vital for establishing trust with stakeholders and regulatory bodies.
- Document and Analyze Results: Maintain thorough documentation of all testing activities, including methodologies, results, and any corrective actions taken. Analyzing these results can provide valuable insights for future product improvements and support regulatory submissions, ensuring that all aspects of the testing process are transparent and traceable.
Conclusion
Navigating the complexities of new product development in medical devices necessitates a strategic approach that encompasses regulatory compliance, user-centered design, advanced technology integration, and thorough testing. By adhering to these best practices, developers can create innovative solutions that not only meet stringent regulations but also enhance user experience and improve patient outcomes.
Key insights from this discussion underscore the importance of:
- Understanding regulatory requirements
- Engaging with users throughout the design process
- Leveraging cutting-edge technologies
- Implementing comprehensive testing protocols
Familiarity with regulations such as the FDA's 21 CFR Part 820 and ISO 13485, alongside the adoption of user-centered design principles, can significantly influence the success of medical devices. Furthermore, the integration of AI, IoT, and advanced materials fosters innovation and enhances functionality, while rigorous testing ensures safety and compliance.
As the landscape of medical device development evolves, it is crucial to stay informed about emerging trends and technologies. Embracing these best practices positions companies to meet current challenges and empowers them to lead in innovation. Ultimately, prioritizing compliance, user experience, and technological advancement will pave the way for the next generation of medical devices, benefiting both patients and healthcare providers alike.
Frequently Asked Questions
Why is understanding regulatory compliance important in medical equipment development?
Understanding regulatory compliance is essential for successfully navigating the complex landscape of medical equipment development, as it ensures adherence to industry regulations and standards.
What specific regulations should I familiarize myself with for medical equipment?
Key regulations include the FDA's 21 CFR Part 820 for quality system regulation and ISO 13485 for quality management systems. Knowing these regulations will guide your creation and development processes.
What is a Design History File (DHF)?
A Design History File (DHF) is a comprehensive document that records the creation and development process of a medical device, including design inputs, outputs, verification, and validation activities. It is vital for compliance submissions and audits.
How can engaging with regulatory bodies benefit my development process?
Engaging with regulatory agencies early in the development process can provide valuable insights and clarify expectations. Scheduling pre-submission meetings can help you discuss your product and gather feedback.
What are design controls and why are they important?
Design controls are systematic measures that ensure the medical device meets user needs and intended uses. They include conducting risk assessments, design reviews, and verification and validation activities throughout development, which are crucial for compliance.
How can I stay informed about changes in compliance requirements?
To stay informed, regularly review updates from regulatory bodies and industry standards organizations. This proactive approach helps ensure ongoing compliance and mitigates risks associated with non-compliance.
List of Sources
- Understand Regulatory Compliance Requirements
- A QMSR State of Mind: FDA Adopts New Inspection Approach for Medical Devices as Quality Management System Regulation Takes Effect | Insights | Ropes & Gray LLP (https://ropesgray.com/en/insights/alerts/2026/02/a-qmsr-state-of-mind-fda-adopts-new-inspection-approach-for-medical-devices)
- Quality Management System Regulation (https://fda.gov/medical-devices/postmarket-requirements-devices/quality-management-system-regulation-qmsr)
- FDA Warning Letter Statistics on Medical Devices in the Past Fiscal Year 2025 - ECA Academy (https://gmp-compliance.org/gmp-news/fda-warning-letter-statistics-on-medical-devices-in-the-past-fiscal-year-2025)
- FDA QMSR & ISO 13485: Key Changes Effective 2026 | IntuitionLabs (https://intuitionlabs.ai/articles/fda-qmsr-iso-13485-changes-2026)
- FDA Implements Quality Management System Regulation for Medical Devices (https://aabb.org/news-resources/news/article/2026/02/04/fda-implements-quality-management-system-regulation-for-medical-devices)
- Incorporate User-Centered Design Principles
- The Key Trends that Will Define Digital Health in 2026. (https://s3connectedhealth.com/blog/the-key-trends-that-will-define-digital-health-in-2026)
- The Importance of User-Centered Design in Developing Medical Software (https://kandasoft.com/blog/user-centered-design-in-developing-medical-software)
- UX design for medical devices: case study ultrasonic cutter (https://interface-design.co.uk/case-studies/ux-ui-design-medical-devices)
- forbes.com (https://forbes.com/councils/forbestechcouncil/2025/03/06/user-centered-research-methods-for-medical-device-design)
- Leverage Advanced Technologies for Innovation
- Top 10 Expert Quotes That Redefine the Future of AI Technology (https://nisum.com/nisum-knows/top-10-thought-provoking-quotes-from-experts-that-redefine-the-future-of-ai-technology)
- AI In Healthcare Statistics By Adoption, Market Size and Facts (2025) (https://electroiq.com/stats/ai-in-healthcare-statistics)
- 9 notable quotes from 1 big day at an epicenter of AI in healthcare – RamaOnHealthcare (https://ramaonhealthcare.com/9-notable-quotes-from-1-big-day-at-an-epicenter-of-ai-in-healthcare)
- Complaint Processing Enhanced by AI in Medical Device Manufacturing (https://usdm.com/resources/case-studies/complaint-processing-enhanced-by-ai-in-medical-device-manufacturing)
- AI in Healthcare 2025 Statistics: Market Size, Adoption, Impact (https://ventionteams.com/healthtech/ai/statistics)
- Conduct Comprehensive Testing and Validation
- medcitynews.com (https://medcitynews.com/2025/10/conducting-a-medical-device-security-risk-assessment)
- consilia-brno.com (https://consilia-brno.com/customised-implementation/system-testing-for-medical-equipment)
- A guide to risk management for medical devices and ISO 14971 (https://medicaldevicehq.com/articles/the-illustrated-guide-to-risk-management-for-medical-devices-and-iso-14971)
- FDA Updates Broaden Wellness and Clinical Decision Support Software Devices Under Enforcement (https://emergobyul.com/news/fda-updates-broaden-wellness-and-clinical-decision-support-software-devices-under-enforcement)





