What Are The Best Heart Rate Monitors of 2021 | Voler Systems
The proliferation of fitness bands and smartwatches has made us more fitness-conscious,...
The U. S. Food and Drug Administration (FDA) has become more proactive and supportive of test development by all comers due to the COVID-19 pandemic — including laboratories and large and small commercial manufacturers — to speed development and to quickly authorize tests that the science supports. In fact, the FDA has worked with over 500 developers since January and continues to work around the clock to authorize over 180 Emergency Use Authorizations (EUAs) for tests. This includes molecular, serology, antigen, and tests with at-home specimen collection indications.
So, what does it take to build FDA approved wearable devices? In this recorded video from the 10X Medical Device Conference, Walt Maclay discussed the issues involved with bringing wearable medical devices from an idea to FDA approval based on his firm’s many experiences. He explores areas including user interface issues, battery life, different sensing technologies, data security, and verification to meet FDA and CE requirements.
Below is an edited transcript of the video:
Voler offers electronic design services for wearable devices and IoT devices. We have helped many firms build medical devices that have been approved by the FDA. Still, here I will be focusing mainly on wearable devices and some of the particular challenges in obtaining accurate physiological measurements, usually the key mission for a wearable medical device. I will explain how battery limitations are major drivers in wearable devices’ design and how to navigate the trade-offs often encountered with limited power. Finally, I will address data security and conclude with some observations on the FDA approval process.
Right now, wearable devices are hot. Fitbit was launched in 2007, but innovations have been coming along, being driven by the need for data since then. Data companies come to us and say, we don’t want to build a piece of hardware, but we need data, so we will have to build one. Hospitals also want to keep patients at home because if patients go back with the same condition within 30 days, the hospitals don’t get paid. But they also don’t want their patients to get sick while staying at home, so what do they do? They monitor their patients at home.
Let’s take a look at ten common parameters doctors want to measure on a patient’s body, how that is done, and some of the challenges in making accurate measurements.
Measuring body temperature seems straightforward since medical thermometers have been in use for more than two centuries. One difficulty is the doctor’s need for measuring body core temperature rather than skin temperature. Skin temperature, particularly on extremities like the wrist, can be different from body core temperature in a cold or hot environment, and other additional measurements may be necessary. For example, if you know that the air temperature is cold, it’s not good to use the value you measure on the skin. If the temperature is moderate, it’s a better time, but if the skin is wet because the person has been exercising, that’s not a good time. The skin could also be wet for other reasons. An accelerometer could detect if the person has been exercising or moving rapidly from exercise. When you combine inputs from several different sensors, the measurement can be much more accurate. This is commonly called sensor fusion.
Contact with the skin is also important because it measures heat flow from inside the body towards the outside surface. If the sensor doesn’t make good contact, the temperature measurement will not be accurate. A wristwatch may not make good contact if it is worn loose; therefore, how people use the device is important.
Motion has been popular for step counts, but it measures other things as well, and manufacturers of motion chips provide the necessary algorithms. For example, gait can be measured and can be an indication of various illnesses. A device on a wrist or ankle can determine if the person is standing, sitting, or walking, and the algorithms for wrist or ankle measurement already exist. Dead reckoning can be helpful to show a person’s actual position and movement direction. Motion sensor chips now have nine axes of motion detection in a single chip. They are good for short term position measurement but lose accuracy over time. If you need to know where somebody is for hours or days, you need GPS, but GPS is power-hungry while motion chips consume very little power.
Heart rate is a crucial health parameter that can be measured in one of three ways:
Pulse oximeters to measure blood Oxygen was developed originally in the 1940s, and the technology is well understood. Two infrared light sources pass light through the body. One of them is sensitive to Oxygen, while both are sensitive to the pulse. When one is subtracted from the other, the pulse measurement is removed. The Oxygen measurement remains. The transmissive type has been in use for a long time. The light passes through a thin part body part like a finger or earlobe or an infant’s foot. Other parts of the body are generally too thick for enough light to pass through; therefore, the alternative is a reflective approach. The amount of light reflected is much smaller than what gets transmitted, and the sensitivity and the accuracy are often a lot less. The challenge is to make them accurate enough to meet FDA requirements.
ECG for the heart, EMG for muscles, and EEG for the brain are measuring electrical signals. This seems straightforward, but you need electrodes, ideally dry electrodes, because applying a wet electrode with a wearable device is inconvenient. For ECG, it’s important to have a separation between the locations of the electrodes. On the chest, I’ve seen one and a half inches work, and that’s small. If you take a look at the Apple Watch, they measure ECG on the wrist, but what you may not have noticed is that you have to reach over with the other hand to touch the watch. The measurement is actually from one hand to the other, far apart; therefore, it doesn’t measure ECG continuously, which is a limitation.
The standard is 12 leads for an ECG., which is what you get in the laboratory or when you go to the doctor. Some companies now claim they are getting equally good results for detecting disease with just two leads. This would typically be on the chest, or alternately from arm to arm by reaching over to touch.
EMG measures the same sort of electrical signal but on muscles. A commonplace to measure is on the forearm. You can detect individual muscles in the forearm and detect which finger is moving from an EMG signal. However, if you don’t have an accurate reference on the arm and are off by a few millimeters, it’s sensing the wrong muscle, and you’re detecting the wrong finger. So how do you position something on the wrist that’s accurate within one or two millimeters? You could put an ink dot there, but that will wear away and will be a problem.
For an EEG, measuring brain signals is the only place to do it on the head. The forehead or the temples are convenient places. There are helmets to do these measurements with a large number of leads. It would be nice if there were another location enabling the device to be worn for a long time. A hat is okay, but not typically indoors.
Respiration is another important parameter, and the standard is to put on a chest strap. Some devices do this, and it’s easy to measure. But a chest strap is inconvenient for many types of wearable devices. Another way of making the measurement is with thoracic impedance. You actually measure the changes in the impedance of the chest as you breathe in and out. This can be quite readily picked up, but the electrodes need to be on the chest. Attempts have been made to do it on the wrist, but I haven’t seen this actually work reliably. The wrist has this big impedance called your arm between it and the chest, so the signal is much weaker, making this method difficult.
Right now, the only way to get an accurate blood pressure measurement is with a cuff on the arm. Some devices work on the wrist, but their accuracy is sensitive to position and questionable. Ideally, you would like to measure it anywhere on the body without an inconvenient cuff. Today, it is commonly done with pulse transit time, measuring the time difference between the heartbeat and when that pulse reaches an extremity. This can be done on the wrist with two electrodes, picking up the ECG signal, which arrives instantly from the heartbeat. A photoplethysmography (PPG) signal arrives when the pulse of blood reaches the extremity. Blood pressure is proportional to the change in the time difference. The difficulty is to get it accurate enough. Some firms claim they’ve gotten enough accuracy to meet FDA requirements for diagnosis, but I haven’t actually seen it. It works fine as an indication that blood pressure has changed. With calibration for each person, the measurement can be accurate. Blood pressure taken with a cuff is entered into the device, and it will give an accurate measurement from then on. Firms are working to improve the algorithm.
Glucose measurement is a prevalent need. Today there are devices with microneedles that are worn as a patch. They don’t actually feel like needles because they go no further than the skin’s outer layer, deep enough to pick up a glucose signal. Wearable patches require calibration with a finger prick once or twice a day because they are not accurate over a long period of time. Good perfusion of blood is necessary for measuring glucose, and unfortunately, the wrist doesn’t have that, although most people would like to wear a device is the wrist. Today, sensors measure blood glucose coupled with pumps to inject insulin and regulate blood glucose, so you can now have a wearable pancreas. There’s been a lot of progress there.
Batteries have been progressing, but slowly. If batteries had progressed like semiconductors over the last 50 years, you would have a battery the size of the head of a pin that would cost a penny and would power your car. We’re not even remotely close and never will be. We’re limited by the space required for the chemical storage of energy. Today’s batteries are about 10% of the ultimate, which would be something like gasoline. However, gasoline has a bit of a problem with safety. I don’t want to carry gasoline in my pocket. Another more efficient option is nuclear energy, but I don’t want to have a nuclear reactor in my pocket either. We will see incremental improvements in batteries in the future, but they will not become smaller.
Every time we design a wearable device or any battery-operated device, people say:
Of course, now we have to make trade-offs.
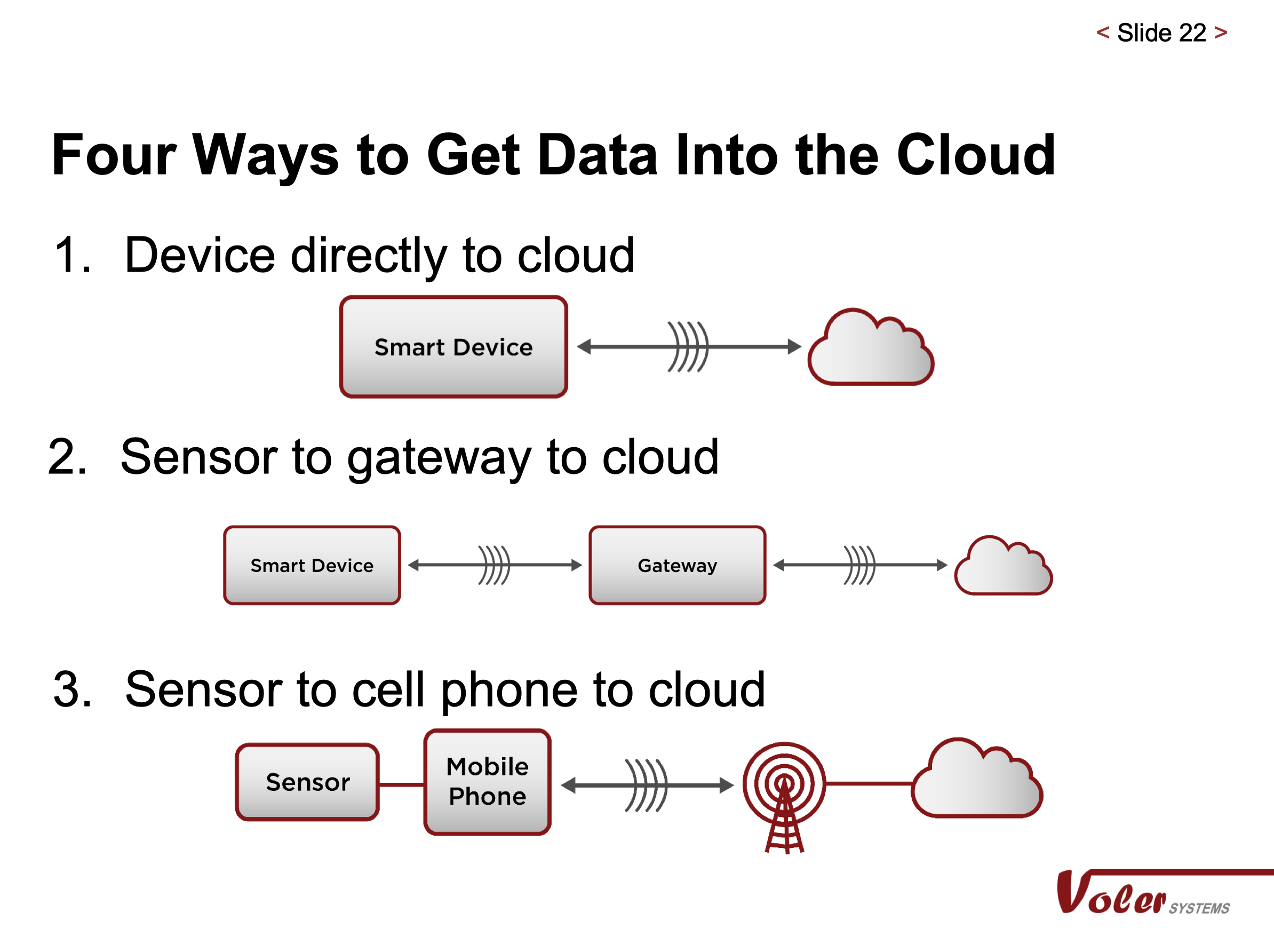
Let’s talk about the impact of limited power. People would like to send data from a wearable device directly to the cloud-like a cell phone. But how long does a large cell phone battery last? Obviously, this isn’t practical for many applications. Another way would be to send the data to a gateway like Wi-Fi, which uses less power. However, most wearable devices are in a third category where they typically use Bluetooth LE to send data to a cell phone to reach the cloud. The wearable device only works when a cell phone is nearby.
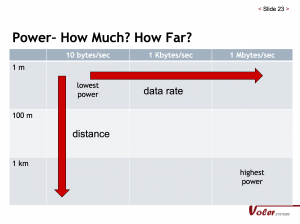
Wireless transmission has a big impact on power usage. In wireless transmission, three trade-offs must be managed: the power required to transmit, data rate, and transmission distance.

Here is a detailed summary of power requirements for popular wireless options. For a full description of the wireless standards, see our Whitepaper Best Wireless Standard for your Application post.
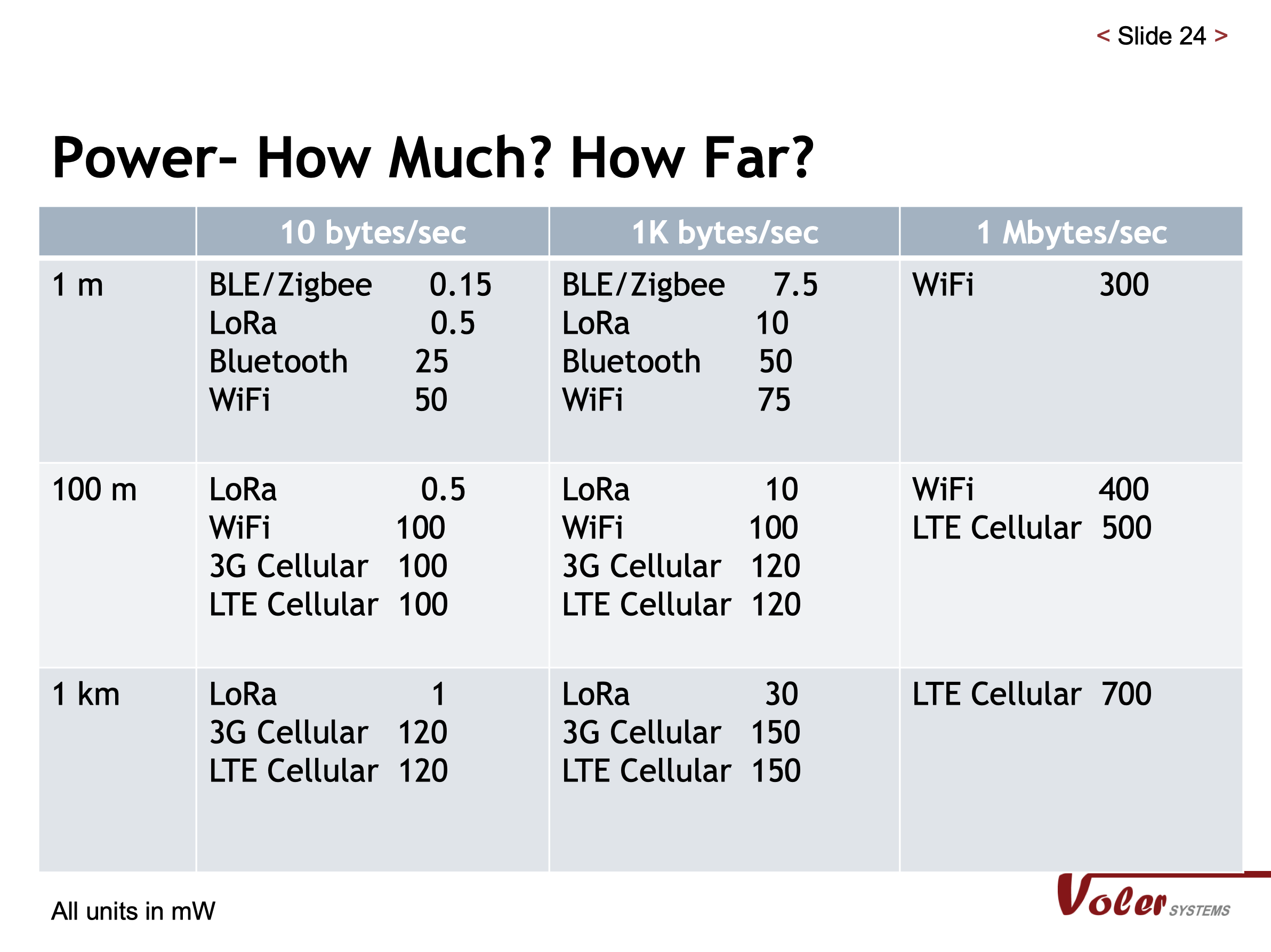
To highlight one option, there is technology out now that enables low-speed data to be sent long distances, but it is not widely available. Soon there will be wearable devices sending data directly to the cloud at nearly the same low energy level as Bluetooth LE.
Taking a look at the first two here, a camera uses a lot of power, 300 milliwatts, which will drain your cell phone quickly, and cell phones have large batteries compared to most wearable devices. The illumination for night time use would almost double that. The police wear cameras, but they require large batteries that are recharged after each shift.
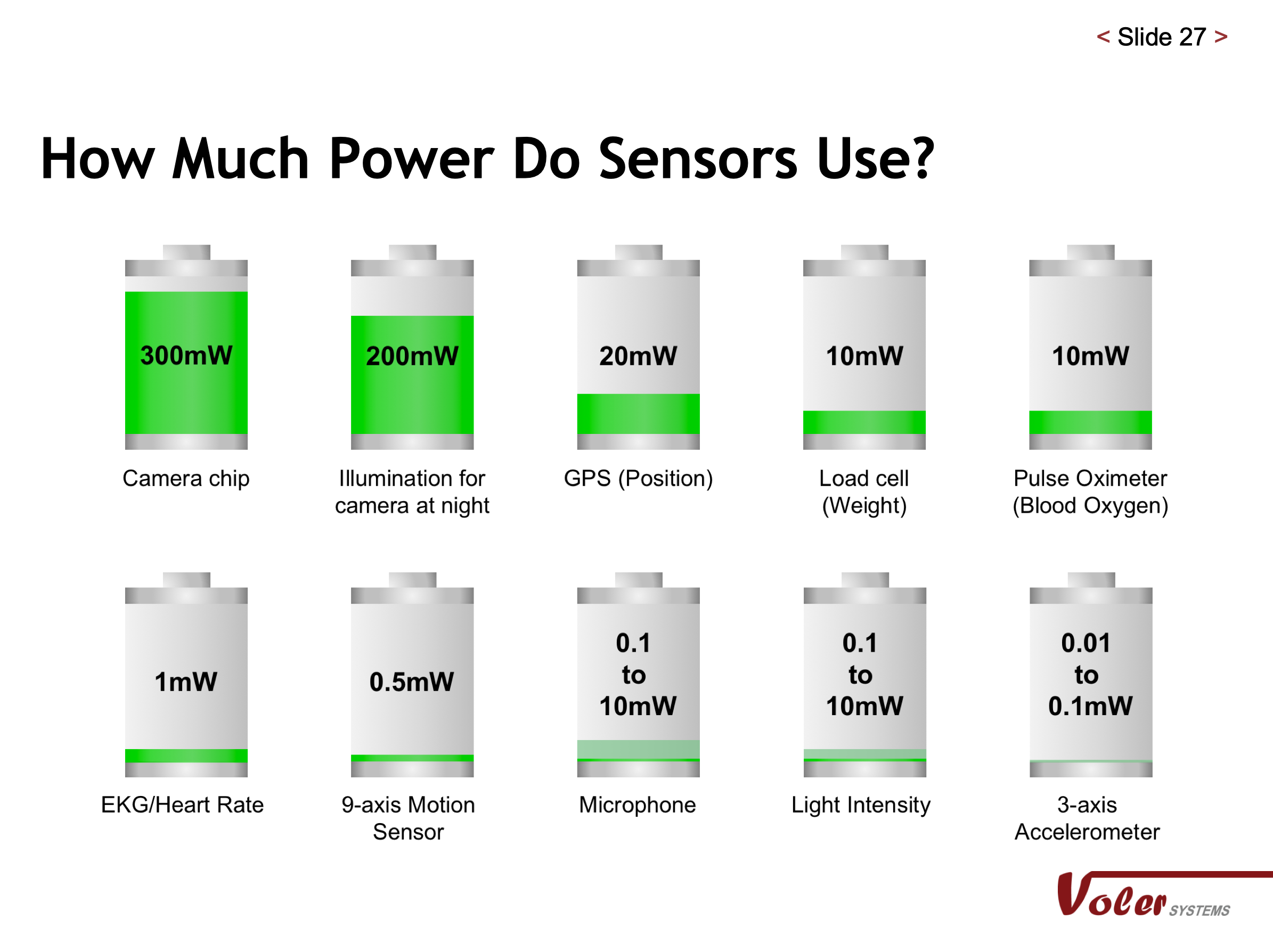
GPS is moderately power-hungry, so you don’t want to run it all the time. A load cell that can measure weight or force is also moderate. Pulse oximeters are a little lower, but you don’t have to run them all the time. How often do you have to know what your oxygen level is? Maybe once an hour in some applications. EKG and heart rate? Now we’re getting to quite a low power. At one milliwatt, that’s 300 times slower than the camera. The nine-axis motion sensor is also deficient. Microphones can be extremely low or moderate. Light intensity is also extremely low to moderate.
But the winner in this is the three-axis accelerometer, which is what Fitbit had to begin with. It uses far less than a milliwatt, just a few microwatts. Devices are often designed to leave the accelerometer running all the time and shut everything else down. When the user moves, it wakes up the processor, which takes more power than the accelerometer. The processor quickly determines if that movement was something important, and if it wasn’t, it goes back to sleep. This is an important way to save power.
Data security is a big deal for wearable devices. The FDA weighed in on this in 2016, so it’s been a while, and the surprising thing is that many people aren’t terribly worried about it. I would expect more of our customers to be more worried about data security. The FDA encourages an end to end security in a guidance document. But a guidance document is not something to be ignored. The data security challenges for a wearable device are much higher than for an endpoint in a fixed location:
It’s easy to have problems with these devices if they are not under the control of a medical professional. Many of these devices can have their software updated over the air. If the device cannot detect where that update is coming from, I can update that device myself. I can put new software on it. Now it’ll do whatever I want it to do. That’s a serious breach of security, and most devices today don’t do a good job in this area.
Fortunately, some companies offer software and hardware that help you solve these security problems, so you don’t have to do it all from scratch. Secure RF has encryption that runs on a tiny processor. Intrinsic-ID and other companies use the random state of RAM at power-up to make a unique key. You don’t have to put the key in the device, it already has it, and every device has a different key. Companies like Secure Push can provide an end-to-end solution for sending data to the cloud, so it’s not as daunting as it might seem, but it still requires great care.
There’s an interesting thing that the FDA has done for apps that run on smartphones and presumably watch. Apps that help people self-manage their disease without providing a specific treatment without a diagnosis are not medical devices. Apps that help patients send data to their medical professionals are not a medical device. Apps that help patients get their data from their health records are not a medical device. Apps that automate tasks for health care workers are not a medical device. However, if you create a wearable device that’s not a phone, and it does the same thing, it may be a medical device. There’s definitely a gray area in the definition of a medical device. It’s effortless to end up making a medical device without realizing it. We help our customers determine if their device needs to be regulated by the FDA or CE.
Thank you for your time.
